- This page was created by volunteers like you!
- Help us make it even better. To learn more about contributing to MEpedia, click here.
- Join the movement
- Visit #MEAction to find support or take action. Donate today to help us improve and expand this project.
- Congratulations!
- MEpedia has got over 30 million views as of August 2022!
Vagus nerve
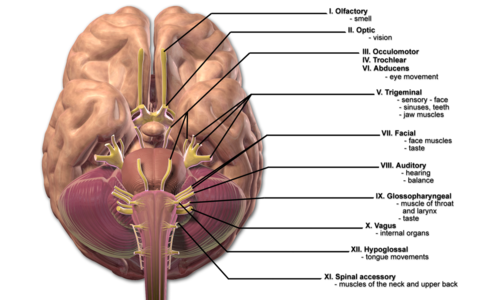
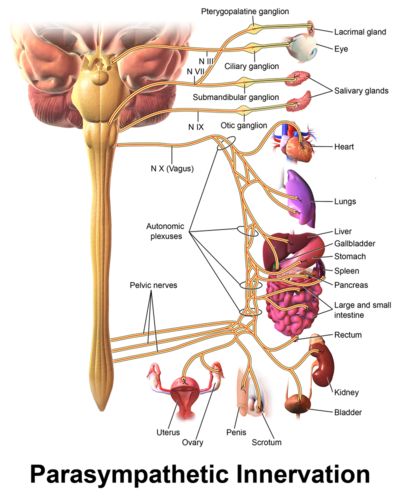
The vagus nerve, also called the tenth cranial nerve, starts in the brain and runs down the trunk of the body, with branches innervating the major organs. A major component of the autonomic nervous system (ANS) and HPA axis, it interfaces with the parasympathetic nervous system (PNS) and helps to regulate the heart, lungs, and the digestive system.[1] It's a bi-directional nerve, meaning it both sends signals from the brain to the organs and the organs send messages back to the brain.[2]
Function[edit | edit source]
The vagus nerve is an important sensor and regulator of basic functions including breathing, heart rate, the relaxation response, the gut-brain connection, and the formation of memories.[3] The motor vagus nerve normally holds inhibitory influence over both systemic inflammation and some autonomic functions such as heart rate. It exerts stimulatory effects on gastric motility, detrusor contraction, pupillary activity, salivatory secretion, and tear secretion and it is also involved in pancreatic exocrine function.
Immune system[edit | edit source]
Because it is a bidirectional nerve, both the afferent (sensory) and efferent (motor) branches have important functions: afferent pathways mediate anti-inflammatory responses via the HPA axis and the release of corticosteroids from the adrenal glands. Efferents pathways mediate anti-inflammatory processes via direct effects on immune cells or through the splenic sympathetic nerve. This system is called the cholinergic anti-inflammatory pathway (CAP).
For example, when the vagus nerve detects pro-inflammatory cytokines such as tumor necrosis factor-alpha or interleukin 1-beta, chemoreceptors in the afferent vagus nerve send a signal into the brainstem that triggers both glial cell activation within the central nervous system as well as the general innate immune response, sometimes called the sickness response. The efferent vagus nerve is responsible for an anti-inflammatory pathway.[4] The vagus nerve speaks directly to the immune system via the neurotransmitter acetylcholine.[5][6][7]
Vagus is thus important for maintaining homeostasis and preventing an overreactive immune response that can cause major injury or death.[4] For example, vagus nerve stimulation (VNS) is being used experimentally as an adjunct treatment for sepsis,[8] which can cause death via a massive cytokine storm.[9]
Autonomic nervous system[edit | edit source]
Vagal tone is a measure of the constitutive output of the motor branch of the vagus nerve. It is frequently measured with the tilt table test because the vagus nerve is responsible for the autonomic changes that allow us to go from lying down to standing up without fainting.
With a loss of vagal tone, both the anti-inflammatory pathway and parasympathetic inhibition over autonomic systems are diminished. According to the vagus nerve infection hypothesis (VNIH), exaggerated sensory vagus nerve signaling leads to loss of vagal tone and therefore a loss of control over inflammation.
Learn more[edit | edit source]
- Dr. Diana Driscoll: Vagus Nerve and POTS/Mast Cell Activation[10]
- 9 Nervy Facts About the Vague Nerve[3]
See also[edit | edit source]
References[edit | edit source]
- ↑ Tewfik, Ted (April 5, 2018). Meyers, Arlen (ed.). "Vagus Nerve Anatomy: Gross Anatomy, Microscopic Anatomy, Natural Variants". Medscape.
- ↑ VanElzakker (December 8, 2015). "Harvard neuroscientist Dr. Michael VanElzakker: chronic fatigue vagus nerve link | Healing Histamine". Healing Histamine. Retrieved August 10, 2018.
- ↑ Jump up to: 3.0 3.1 Rosenfeld, Jordan (July 2, 2015). "9 Fascinating Facts About the Vagus Nerve". Mental Floss. Retrieved August 10, 2018.
- ↑ Jump up to: 4.0 4.1 Pavlov, Valentin A; Wang, Hong; Czura, Christopher J; Friedman, Steven G; Tracey, Kevin J (2003). "The Cholinergic Anti-inflammatory Pathway: A Missing Link in Neuroimmunomodulation". Molecular Medicine. 9 (5–8): 125–134. ISSN 1076-1551. PMID 14571320.
- ↑ "Direct Route From The Brain To The Immune System Discovered". ScienceDaily. October 24, 2007. Retrieved August 10, 2018.
- ↑ Gallagher, Laura (February 24, 2015). "Scientists uncover new role for neurotransmitter that helps fight infection | Imperial News | Imperial College London". Imperial News. Retrieved August 10, 2018.
- ↑ Darby, Matthew; Schnoeller, Corinna; Vira, Alykhan; Culley, Fiona; Bobat, Saeeda; Logan, Erin; Kirstein, Frank; Wess, Jürgen; Cunningham, Adam F (January 28, 2015). "The M3 Muscarinic Receptor Is Required for Optimal Adaptive Immunity to Helminth and Bacterial Infection". PLOS Pathogens. 11 (1): e1004636. doi:10.1371/journal.ppat.1004636. ISSN 1553-7374. PMC 4309615. PMID 25629518.
- ↑ Wang, Da-Wei; Yin, Yi-Mei; Yao, Yong-Ming (September 2, 2016). "Vagal Modulation of the Inflammatory Response in Sepsis". International Reviews of Immunology. 35 (5): 415–433. doi:10.3109/08830185.2015.1127369. ISSN 1563-5244. PMID 27128144.
- ↑ Karbian, Netanel; Abutbul, Avraham; el-Amore, Raja; Eliaz, Ran; Beeri, Ronen; Reicher, Barak; Mevorach, Dror (July 15, 2020). "Apoptotic cell therapy for cytokine storm associated with acute severe sepsis". Cell Death & Disease. 11 (7): 1–14. doi:10.1038/s41419-020-02748-8. ISSN 2041-4889.
- ↑ "Dr. Diana Driscoll interview: vagus nerve and POTS/mast cell activation | Healing Histamine". Healing Histamine. January 12, 2016. Retrieved August 10, 2018.

