- This page was created by volunteers like you!
- Help us make it even better. To learn more about contributing to MEpedia, click here.
- Join the movement
- Visit #MEAction to find support or take action. Donate today to help us improve and expand this project.
- Congratulations!
- MEpedia has got over 30 million views as of August 2022!
Brain fog
Brain fog manifests as impaired working memory and concentration accompanied by difficulty processing complex information.[1]
It is a type of cognitive impairment experienced by ME/CFS patients. Fibromyalgia patients often refer to it as "fibro fog".[2]
Causes[edit | edit source]
Brain fog is a common symptom of Myalgic Encephalomyelitis/Chronic Fatigue Syndrome, but can also be caused - or linked to - other illnesses:
- during chemotherapy, the mild cognitive impairment is often called "chemo brain" or "chemo fog"[3]
- depression - concentration problems may be described as brain fog[4]
- Ehlers-Danlos syndrome (EDS) patients may use the term brain fog to refer to the "inability to focus and maintain concentration" that is common in people with EDS, although ME/CFS is also common in people with EDS[5]
- the endocrine disorder hypoparathyroidism, which also causes mood problems[6]
- brain fog is common in people with fibromyalgia, and is often referred to as "fibro fog"[2]
- gluten sensitivity[7] or celiac disease[8]
- hepatitis C virus[9]
- hypocalcemia - low levels of calcium in the blood, which also causes fatigue and many other symptoms[10]
- brain fog may be described by people with Ehlers-Danlos syndrome (EDS) as the "inability to focus and maintain concentration" that common in people with EDS, although ME/CFS is also common in people with EDS[11]
- Lyme disease patients may use the term brain fog to describe an impairment in thinking[12]
- postural orthostatic tachycardia syndrome (POTS) or other forms of orthostatic intolerance cause brain fog, "impaired cognition" and many other symptoms occur when a person stands or moves to an upright position[13][14]
- brain fog may be used to describe memory impairment resulting from concussion or traumatic brain injury[15]
- sarcoidosis-associated brain fog, which also causes fatigue[16]
- Sjögren's syndrome[17]
- Postorgasmic illness syndrome
- Long Covid
Presentation[edit | edit source]
Prevalence[edit | edit source]
- Katrina Berne reports a prevalence of 75-100% for confusion and inability to think clearly.[18]
Symptom recognition[edit | edit source]
Notable studies[edit | edit source]
- 2013, What is brain fog? An evaluation of the symptom in postural tachycardia syndrome[19]
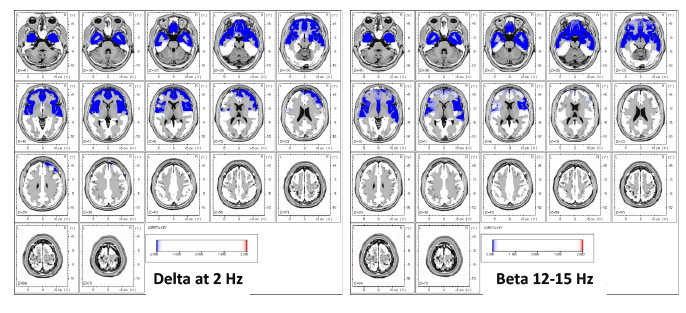
- 2016, qEEG / LORETA in Assessment of Neurocognitive Impairment in a Patient with Chronic Fatigue Syndrome: A Case Report[20]
Our case study confirmed the pattern of dysregulation in the cortex reviewed in the introduction. Furthermore, since both periods of phase shift/lock durations were found to be significantly shorter, that might contribute to an increased rate of phase reset, also seen in our data. Phase reset deregulation--phase locking periods being too brief and phase reset happening too often—appear to be consistent with the associated lower rate of information processing and reaction times found in the ME and CFS literature. These deregulated states represent the brain during nonoptimal functioning, rendering it inefficient for most types of information processing functioning, whether it is executive functioning, memory, perceptual reasoning or information processing speed. When phase lock is significantly less than normal, as in this data set, the ability of the brain to sustain commitment of resources to mediate different functions is severely compromised. Phase shift duration in this data is also hypoactive, meaning that significantly less neurons are being recruited to perform a function than normal. The results here indicate slowed verbal comprehension, executive functions, perceptual reasoning, processing speed and memory, the sum total of which is known as cognitive impairment.[20]
- 2018, Cognitive Impairment in Fibromyalgia: A Meta-Analysis of Case–Control Studies[21] - (Abstract)
Possible causes[edit | edit source]
Potential treatments[edit | edit source]
Learn more[edit | edit source]
- 2013, Brain Fog in ME/CFS: What's Going On? - Solve ME/CFS
- 2016, Case Study: “Brain Fog” in CFS can be seen in qEEG/Loreta - #MEAction
- 2018, Study Identifies the Types of Cognitive Dysfunction That Are Most Prevalent in Fibromyalgia
According to the Marshall Pathogenesis, cognitive dysfunction is caused by microbes. More severe forms of cognitive dysfunction are seen in diseases such as Alzheimer's, diseases for which there is strong evidence of a bacterial etiology. Often associated with chronic fatigue syndrome,1) cognitive dysfunction is also seen in patients with multiple sclerosis,2) depression,3) fibromyalgia,4) and dozens of others diseases.[22]
- 2024, Long Covid ‘brain fog’ may be due to leaky blood-brain barrier, study finds The Guardian
See also[edit | edit source]
- Aphasia
- Blood-brain barrier
- Cognitive dysfunction
- Dyscalculia
- Dysphasia
- Fibromyalgia
- Long COVID
- ME/CFS
- Memory problems
- Word-finding problems
References[edit | edit source]
- ↑ "Brain Fog in ME/CFS: What's Going On? - Solve ME/CFS Initiative". Solve ME/CFS Initiative. Retrieved August 10, 2018.
- ↑ Jump up to: 2.0 2.1 Abril, Andy; Bruce, Barbara K. (September 24, 2019). Mayo Clinic Guide to Fibromyalgia: Strategies to Take Back Your Life (= ed.). Simon and Schuster. p. 69. ISBN 978-1-893005-49-5.
- ↑ McKay, Judith; Schacher, Tamera (May 2009). The Chemotherapy Survival Guide: Everything You Need to Know to Get Through Treatment. New Harbinger Publications. p. 163. ISBN 978-1-57224-621-8.
- ↑ Alpert, Jack N. (November 27, 2018). The Neurologic Diagnosis: A Practical Bedside Approach. Springer. p. 50. ISBN 978-3-319-95951-1.
- ↑ Overeem, Sebastiaan; Reading, Paul (September 24, 2018). Sleep Disorders in Neurology: A Practical Approach. John Wiley & Sons. p. 4. ISBN 978-1-118-77726-8.
- ↑ Camacho, Pauline M. (February 22, 2019). Metabolic Bone Diseases: A Case-Based Approach. Springer. ISBN 978-3-030-03694-2.
- ↑ Ukleja, Andrew (February 7, 2018). Nutritional Management of Gastrointestinal Disease, an Issue of Gastroenterology Clinics of North America. Elsevier Health Sciences. p. 141. ISBN 978-0-323-58155-4.
- ↑ Levenson, James L.; Ferrando, Stephen J. (October 18, 2016). Clinical Manual of Psychopharmacology in the Medically. III (2nd ed.). American Psychiatric Pub. p. 142. ISBN 978-1-58562-501-7.
- ↑ Miyamura, Tatsuo; Lemon, Stanley M.; Walker, Christopher M.; Wakita, Takaji (October 28, 2016). Hepatitis C Virus II: Infection and Disease. Springer. p. 168. ISBN 978-4-431-56101-9.
- ↑ Papadakis, Maxine A.; McPhee, Stephen J.; Rabow, Michael W. (September 9, 2019). CURRENT Medical Diagnosis and Treatment 2020 (59 ed.). McGraw Hill Professional. pp. 915, 1169. ISBN 978-1-260-45529-8.
- ↑ Overeem, Sebastiaan; Reading, Paul (September 24, 2018). Sleep Disorders in Neurology: A Practical Approach. John Wiley & Sons. p. 4. ISBN 978-1-118-77726-8.
- ↑ Georgiev, Vassil St (July 6, 2009). National Institute of Allergy and Infectious Diseases, NIH: Volume 2: Impact on Global Health. Springer Science & Business Media. ISBN 978-1-60327-297-1.
- ↑ Evans, Randolph W. (August 2, 2016). Case Studies in Neurology, An Issue of Neurologic Clinics. Elsevier Health Sciences. p. 538. ISBN 978-0-323-45980-8.
- ↑ DePace, Nicholas L.; Colombo, Joseph (August 1, 2019). Clinical Autonomic and Mitochondrial Disorders: Diagnosis, Prevention, and Treatment for Mind-Body Wellness. Springer. p. 515. ISBN 978-3-030-17016-5.
- ↑ Louis, Elan D.; Mayer, Stephan A.; Rowland, Lewis P. (August 31, 2015). Merritt's Neurology. Lippincott Williams & Wilkins. ISBN 978-1-4963-2107-7.
- ↑ Lisak, Robert P.; Truong, Daniel D.; Carroll, William M.; Bhidayasiri, Roongroj (June 13, 2016). International Neurology. John Wiley & Sons. p. 97. ISBN 978-1-118-77736-7.
- ↑ Hochberg, Marc C.; Silman, Alan J.; Smolen, Josef S.; Weinblatt, Michael E.; Weisman, Michael H. (June 24, 2014). Rheumatology. Elsevier Health Sciences. p. 304. ISBN 978-0-7020-6303-9.
- ↑ Berne, Katrina (December 1, 1995). Running on Empty: The Complete Guide to Chronic Fatigue Syndrome (CFIDS) (2nd ed.). Hunter House. p. 59. ISBN 978-0897931915.
- ↑ Ross, A.J.; Medow, M.S.; Rowe, P.C.; Stewart, J.M. (2013). "What is brain fog? An evaluation of the symptom in postural tachycardia syndrome". Clinical Autonomic Research : Official Journal of the Clinical Autonomic Research Society. 23 (6): 305–311. doi:10.1007/s10286-013-0212-z.
- ↑ Jump up to: 20.0 20.1 20.2 Zinn, Marcie; Zinn, Mark; Jason, Leonard (2016). "qEEG / LORETA in Assessment of Neurocognitive Impairment in a Patient with Chronic Fatigue Syndrome: A Case Report" (PDF). Clinical Research: Open Access. 2 (1). doi:10.16966/2469-6714.110.
- ↑ Wu, Yu-Lin; Huang, Chun-Jen; Fang, Su-Chen; Ko, Ling-Hsin; Tsai, Pei-Shan (2018). "Cognitive Impairment in Fibromyalgia: A Meta-Analysis of Case–Control Studies". Psychosomatic Medicine. 80 (5): 432–438. PMID 29528888.
- ↑ Jump up to: 22.0 22.1 "Cognitive dysfunction (brain fog) (MPKB)". mpkb.org. Retrieved August 28, 2018.

