- This page was created by volunteers like you!
- Help us make it even better. To learn more about contributing to MEpedia, click here.
- Join the movement
- Visit #MEAction to find support or take action. Donate today to help us improve and expand this project.
- Congratulations!
- MEpedia has got over 30 million views as of August 2022!
Autopsy in Myalgic Encephalomyelitis
Brain[edit | edit source]
Enteroviruses[edit | edit source]
Three post-mortem studies have found enterovirus infections in the brains of myalgic encephalomyelitis / chronic fatigue syndrome patients:
McGarry 1994 study[edit | edit source]
In 1994 McGarry, Gow and Behan published an autopsy study[1] of a 30 year old female who had ME/CFS for 5 years and died of complications after a suicide attempt. Brain samples were obtained from the frontal, temporal, parietal and occipital cortices and from the mid-brain, hypothalamus and brainstem. Using PCR, enteroviral RNA was found in the heart, muscles, hypothalamus and brainstem of this patient. The RNA showed an 83% homology to coxsackie B3 virus. Control tissue samples taken from 8 brains (four patients who died of cerebrovascular diseases, and four others who had depression and died by suicide) showed no evidence of enteroviral RNA.
Richardson 2001 study[edit | edit source]
The John Richardson 2001 study[2] examined the brain tissues of a male ME/CFS patient who died from suicide by hanging. This patient had high titers to coxsackie B1 virus, and also titers to coxsackie B4 virus. Brain tissue samples were sent to Professor James Mowbray, who used immunoperoxidase staining with monoclonal antibody D8/1 to detect enteroviral VP1 protein. Enterovirus VP1 protein was found in fibroblasts in the adventitia of small blood vessels in the cerebral cortex, and there was a patchy distribution of the VP1 protein in a small fraction of the glial cells. Note that most glial cells are astrocytes, and one study found coxsackie B virus can create a persistent infection in human astrocyte cells lines,[3] and another found coxsackie B virus can replicate in the astrocytes of mice brains.[4]
Chia 2015 study[edit | edit source]
A | 2015 study[5] by John Chia looked at the brain tissues of another ME/CFS patient, a 23 year old male with high titers to echovirus 11 who who committed suicide 6 years after the onset of symptoms. Using Western blot, Chia found evidence of enterovirus infection in the pontomedullary junction and midbrain (both are in the brainstem), medial temporal lobe, lateral frontal cortex, occipital lobe and cerebellum. And by RT-PCR, Chia found enterovirus RNA in the frontal cortex, pontomedullary junction. When the virus was sequenced, they found a 92% homology to CVB2, and about 86% to echovirus 30.[6]
Interestingly enough, the first time Chia used RT-PCR to find enterovirus RNA in this patient's brain tissue, he got a negative result. But Chia remembered a phenomenon whereby viral RNA may bind to chromosomal DNA, preventing RT-PCR from detecting the RNA. So Chia used the DNase enzyme to digest the chromosomal DNA in the brain tissue, and after doing this, he was able to find enterovirus RNA in the frontal cortex and pontomedullary junction.[7]
Dr Chia points out that an enterovirus infection in the stomach can travel along the vagus nerve (via reverse axonal transport) and reach the brainstem in around 3 days. In this way, the virus can bypass the blood-brain barrier, and enter into the brainstem, infecting the brain.[8] Chia also questions the common wisdom that in brain infection, you will find the virus in the cerebrospinal fluid: he points out this is not always true in the case of enterovirus, because even in acute enterovirus 71 infection, only 5% of the cerebrospinal fluid samples are positive, and ME/CFS does not involve an acute brain infection, but rather a chronic one. Dr Chia points out that in ME/CFS, enterovirus infections are found in the tissues, not really so much in the blood and fluids.[9] This is because the persistent enterovirus infections found in the tissues of ME/CFS patients are of the aberrant non-cytolytic enterovirus form.
The following table summarizes the areas of the brains of ME/CFS patients in which enterovirus infection was found post-mortem:
| Brain Study | Date | Enterovirus Infected Areas in Red | Enterovirus Testing Method | Areas Of Brain Found Infected With Enterovirus |
|---|---|---|---|---|
| McGarry, Gow and Behan [1] | 1994 | 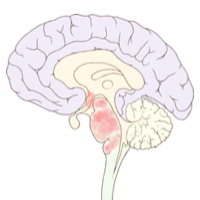
|
PCR | Hypothalamus and brainstem. |
| John Richardson [2] | 2001 | 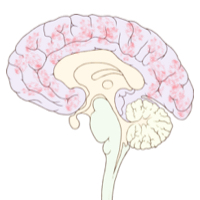
|
VP1 protein stain | Fibroblasts in the adventitia of small blood vessels in the cerebral cortex, and also in a small fraction of the glial cells. |
| John Chia [5] | 2015 | 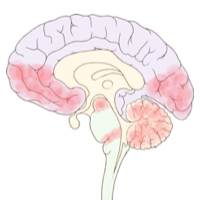
|
Western blot | Pontomedullary junction and midbrain (both are in the brainstem), medial temporal lobe, lateral frontal cortex, occipital lobe and cerebellum. |
| RT-PCR | Frontal cortex, pontomedullary junction. |
Herpesviruses[edit | edit source]
Prusty 2022 study[edit | edit source]
Dr Bhupesh K Prusty and colleagues in a post-mortem study found evidence of active HHV-6 infection in the brain tissues of 2 out of 3 ME/CFS patients, whereas none of the 3 controls had active HHV-6 infection in their brain tissues.[10]
Spine[edit | edit source]
Inflammation of the dorsal root ganglia (ganglionitis) has been found in the autopsies of several very severely ill myalgic encephalomyelitis patients including Lynn Gilderdale, Sophia Mirza and Merryn Crofts.[citation needed]
Other post-mortem findings[edit | edit source]
The results of the autopsies of four ME/CFS patients were presented at the International Science Symposium on ME/CFS, 2010, Bond University, Australia.[11] These autospy studies were not looking for enterovirus, but examined the general features of the brain and nervous system.
- A 32 year old male had ME/CFS for 20 years and died of suicide by medication overdose. The autopsy showed excess corpora amylacea in the spinal cord and brain. There were intermediate filaments closely related to glial cells, and maybe within the glia rather than the axons. No evidence of ganglionitis. (EBV negative).
- A 32 year old female had ME/CFS for 5 years. She refused medical help, was bedridden and refused food and water. She finally died of renal failure. The autopsy showed a focal chronic inflammatory infiltrate (T8 lymphocyes) in the dorsal root ganglia. (EBV negative).
- A 43 year old female arranged for assisted suicide in Switzerland by barbiturate overdose. The brain showed global ischemia, but this was likely due to the drugs used. Dorsal root ganglia showed mild excess of lymphocytic nodules of nageotte but with no obvious inflammation, but this could represent a subtle chronic inflammatory state.
- A 31 year old female with ME/CFS may have died from opiate ingestion. She had toxic demyelination with spinal subarachnoid hemorrhage, but she was on warfarin. There was some mild possible chronic ganglionitis.
Autopsies of two patients who died from other causes several months after contracting ME/CFS in the 1955 Royal Free hospital outbreak revealed distinct brain abnormalities in one case, but not in the other:[12]
- A 32 year old female had had ME/CFS for 7 months at the time of death (due to barbiturate poisoning). A brain post-mortem showed small grey or yellowish plaques in the white matter of the cerebral hemispheres (mainly paraventricular in distribution), in the brain stem, and in the spinal cord (particularly in the cervical segment). Microscopic brain tissue examination showed multiple areas of demyelination with associated microglia and astrocyte proliferation and gliosis. One section from the hypothalamus showed intense perivascular cuffing (accumulation of lymphocytes or plasma cells), which it was concluded could be due to viral encephalitis, or due an unusual reaction associated with the white matter sclerosis .
- The other Royal Free epidemic ME/CFS patient autopsied was found to have septicemia, clostridial peritonitis and ovarian carcinoma with multiple metastases. Microscopic examination of the brain, spinal cord and peripheral nerves showed no abnormalities except for those attributable to the septicemia or the disseminated carcinoma.
See also[edit | edit source]
- Coxsackie B virus
- Echovirus
- Enterovirus
- Enterovirus infection studies
- John Chia
- John Richardson | last4
- Non-cytolytic enterovirus | last4
- Peter Behan
Links[edit | edit source]
Full text versions of the enterovirus post-mortem brain studies here.
References[edit | edit source]
- ↑ Jump up to: 1.0 1.1 McGarry, F; Gow, J; Behan, PO (1994). "Enterovirus in the chronic fatigue syndrome". Ann Intern Med. 120 (11): 972–3. PMID 8172448.
- ↑ Jump up to: 2.0 2.1 Richardson, J. (2001). "Viral Isolation from Brain in Myalgic Encephalomyelitis". Journal of Chronic Fatigue Syndrome. 9 (3–4): 15–19. doi:10.1300/J092v09n03_03. ISSN 1057-3321.
- ↑ Zhang, Xiaowei; Zheng, Zhenhua; Shu, Bo; Liu, Xijuan; Zhang, Zhenfeng; Liu, Yan; Bai, Bingke; Hu, Qinxue; Mao, Panyong (November 15, 2013). "Human Astrocytic Cells Support Persistent Coxsackievirus B3 Infection". Journal of Virology. 87 (22): 12407–12421. doi:10.1128/JVI.02090-13. ISSN 0022-538X. PMC 3807905. PMID 24027313.
- ↑ Zeng, Jun; Wang, Gefei; Li, Weizhong; Zhang, Dangui; Chen, Xiaoxuan; Xin, Gang; Jiang, Zhiwu; Li, Kangsheng (2013). "Induction of cytopathic effect and cytokines in coxsackievirus B3-infected murine astrocytes". Virology Journal. 10 (1): 157. doi:10.1186/1743-422x-10-157. ISSN 1743-422X. PMC 3680086. PMID 23693026.
- ↑ Jump up to: 5.0 5.1 "Chronic enterovirus infection in a patient with myalgic encephalomyelitis / chronic fatigue syndrome (ME/CFS) – clinical, virologic and pathological analysis. John Chia, David Wang, Andrew Chia, Rabiha El-Habbal. 2015. Presented at the 19th International Picornavirus Meeting, 2016".
- ↑ "Dr John Chia's presentation at the Invest in ME London Conference 2015 (available on DVD), timecode 27:32".
- ↑ "Dr John Chia's presentation at the Invest in ME London Conference 2015 (available on DVD), timecode 26:46".
So when we did our RT-PCR again it's completely negative. That's the positive control here, negative control here. Then we remembered one phenomena: so we actually use the DNase to try to digest any chromosomal DNA off this RNA. We think they are attached like this. Then we repeated the RT-PCR: then we saw the band here, for the pontomedullaryjunction, and this one's the frontal cortex, here's the positive strand, the positive control and negative control. Then we sequenced it: this is our top band for the pontomedullary junction, OK, and that's clearly different from the positive control. And that was about 92% homology to CVB2, about 86% to echovirus 30.
- ↑ "Dr John Chia's presentation at the State of Knowledge Workshop on ME/CFS, National Institutes of Health, April 2011, day 1, part 1, timecode 2:20".
- ↑ "Dr John Chia's presentation at the State of Knowledge Workshop on ME/CFS, National Institutes of Health, April 2011, day 1, part 2, timecode 9:33".
- ↑ Kasimir, Francesca; Toomey, Danny; Liu, Zheng; Kaiping, Agnes C.; Ariza, Maria Eugenia; Prusty, Bhupesh K. (2022). "Tissue specific signature of HHV-6 infection in ME/CFS". Frontiers in Molecular Biosciences. 9. doi:10.3389/fmolb.2022.1044964/full. ISSN 2296-889X.
- ↑ "Pathology of Chronic Fatigue Syndrome: Pilot Study of Four Autopsy Cases. DG O'Donovan, T Harrower, S Cader, LJ Findley, C Shepherd, A Chaudhuri. Presented at the International Science Symposium on ME/CFS, 2010, Bond University, Australia".
- ↑ Crowley, Nuala; Nelson, Merran; Stovin, Sybille (March 1957). "Epidemiological aspects of an outbreak of encephalomyelitis at the Royal Free Hospital, London, in the summer of 1955". The Journal of Hygiene. 55 (1): 102–122. ISSN 0022-1724. PMC 2217874. PMID 13416578.

